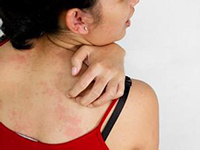
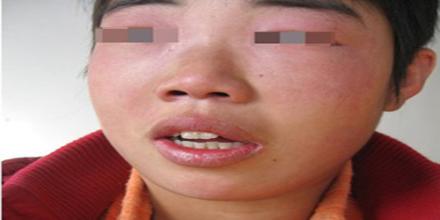
利妥昔单抗可作为皮肌炎的一线治疗药物
这里报道一例20岁,女孩,确诊为皮肌炎。给予激素治疗有效,但是必需要高剂量激素下维持,减量后病情有反复。后加用利妥昔单抗治疗后,病情临床及生物学上显明改善,且无复发。武警总医院神经内科吴士文
Rheumatol Int. 2010 Mar 26. [Epub ahead of print]
Rituximab as a first-line agent for the treatment of dermatomyositis.Haroon M, Devlin J.
Department of Rheumatology, Waterford Regional Hospital, Waterford, Republic of Ireland, mharoon301@hotmail.com.
B cells may play a pivotal role in the pathophysiology of DM, and reports have claimed that targeting B cells is a viable treatment option in patients with dermatomyositis. A 20-year-old girl presented in October 2007, with few weeks' history of proximal muscle weakness. Gottron's papules were noted on her knuckles. She had normal inflammatory markers and negative autoantibody screen. Her CPK was 7,000 U/L (normal range 0-170) with an LDH of 1,300 U/L (normal range 266-500). EMG and muscle biopsy was consistent with active myositis. She had normal pulmonary function tests. HRCT showed no interstitial lung disease. She was started with 60 mg glucocorticoids (1 mg/kg), with a good clinical response. However, any attempt to taper down the steroid dose led to recurrence of her symptoms. The options of available immunosuppressive therapies, including the experimental usage of rituximab, were discussed with her; averse to long-term systemic treatments, she opted to try a course of rituximab. She had rituximab 1,000 mg on days 0 and 14, and her glucocorticoids were tapered in next few weeks. Now, 24 months since her rituximab infusions, she remains in complete clinical and biochemical remission and is naïve to other immunosuppressive agents apart from glucocorticoids and rituximab. Depleting peripheral B cells with rituximab (one course) in our patient has led not only to complete resolution of muscle and skin disease (induction) but also remains off all immunosuppressives including glucocorticoids.
- 上一篇:甲氨蝶呤是什么药,如何使用才安全?
- 下一篇:什么是无肌病性皮肌炎?
相关文章
- 西药如何治疗皮肌炎疾病
- 皮肌炎的两大主要药物疗法
- 皮肌炎吃什么药
- 皮肌炎药物治疗
- 治疗皮肌炎的药物
- 皮肌炎中药疗法有什么
- 治疗皮肌炎有什么好的药方吗?
- 中药治疗皮肌炎
- 治皮肌炎的药膏有哪些?
- 皮肌炎的治疗药物是什么
- 治疗皮肌炎有什么药方呢?
- 皮肌炎中药治疗的方法有什么?
- 热点排行
免费提问